Category - Physician Careers

How to serve a medical mission
February 13th, 2024 Interested in serving a medical mission? Learn everything you need to know to get started — from choosing where to go to what to expect when you get there.
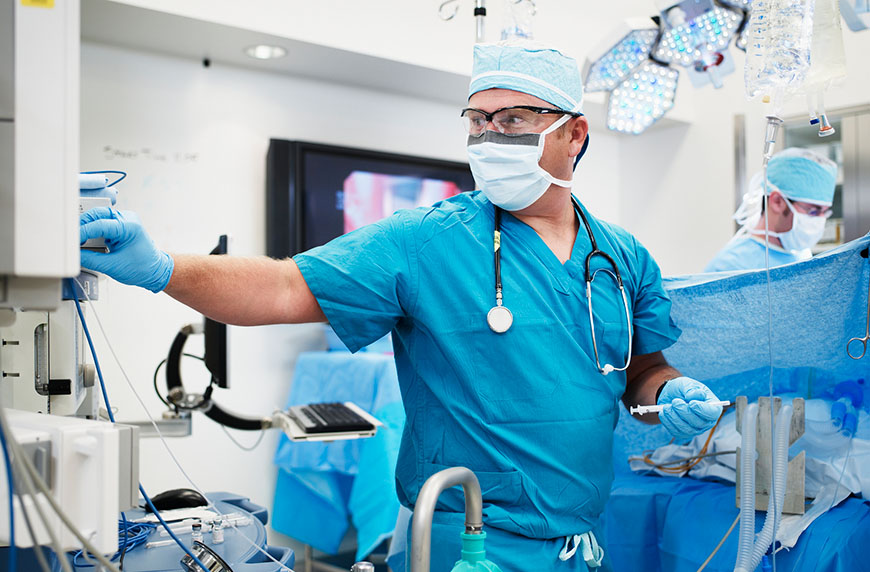
A physician’s guide to working as an independent contractor: Unique ways to work locum tenens
December 11th, 2023 This physician’s guide to working as an independent contractor can help you learn about the variety of ways doctors can work locum tenens.
How does locum tenens pay and salary work for physicians?
October 31st, 2023 Answers to commonly asked questions about locum tenens pay and salary for physicians.
10 best cities for physicians in the U.S. in 2023
September 6th, 2023 If you're a physician looking for a city to settle down in, here are 10 great cities to check out.